Heart
During the Autumn of 2008 I was experiencing brief episodes in which my heart pulse rate was abnormally slow. I felt a weakness and internal oddities comparable in intensity to simple hunger. It was with a pulse oximeter that I was able to tie those symptoms to a slow pulse rate. More expensive tests during December, including a heart echo exam (ultrasound) and an event monitor (portable EKG), failed to show anything unusual. I had not had a known heart irregularity episode since 9 December.
On 12 January 2009, the day after my 64th birthday, we scheduled another test, this time at the hospital cardiac unit using a tilt table test. I was told to have no food after my early (5 AM) breakfast and to drink only water. The test was scheduled for 1:30 PM.
An unexpected snowfall occurred that morning, dropping about a half foot of snow with 0.36 inches of water content. I spent about two hours shoveling snow from my driveway so that the cars could get out. Such significant exercise is not unusual for me, for I seek out opportunities for such steady labor. I did not feel the need to drink water during the morning even though it was allowed. Neither did I feel hungry, even at 1 PM, maybe because of the big dinner the night before during our delayed Christmas celebration with family. Even so, my body was apparently stressed from the exercise and lack of food.
The tilt table test is generally boring. I was strapped down on a table which was later raised to near vertical (70 degrees) at the start of the test. EKG electrodes were placed around my chest and an IV of saline solution was injected into my left arm. A nurse took blood pressure readings every 5 minutes. When the table was raised my feet were flat against a rigid plate at the end of the table and took most of my weight. The straps were to keep me from falling over if I lost consciousness. I was told that some patients go for about 45 minutes before the test ends.
So I just rested that way for more than 20 minutes. Eventually I started to feel odd, as with my slow-heart symptoms, a little woozy, and then a prelude to a faint. I told the nurse as my feelings changed. She sped up the blood pressure readings. It was then about 24 minutes into the test. I really did faint and remembered nothing about what happened next until I woke up with numerous people around me and the bed was back in a horizontal position.
The EKG trace recorded what happened, as shown in these illustrations. The horizontal scale is that 5 small squares span 1 second of time. The four graphs of my heart's electrical activity are sequential, continued on the next line down. The first line shows my heart pulse rate slowing down to as little as 36 pulses/minute, where 60 and faster are normal. That was the same symptom that I had seen months earlier, and I was delighted afterwards that at last there was a test that revealed such an irregularity.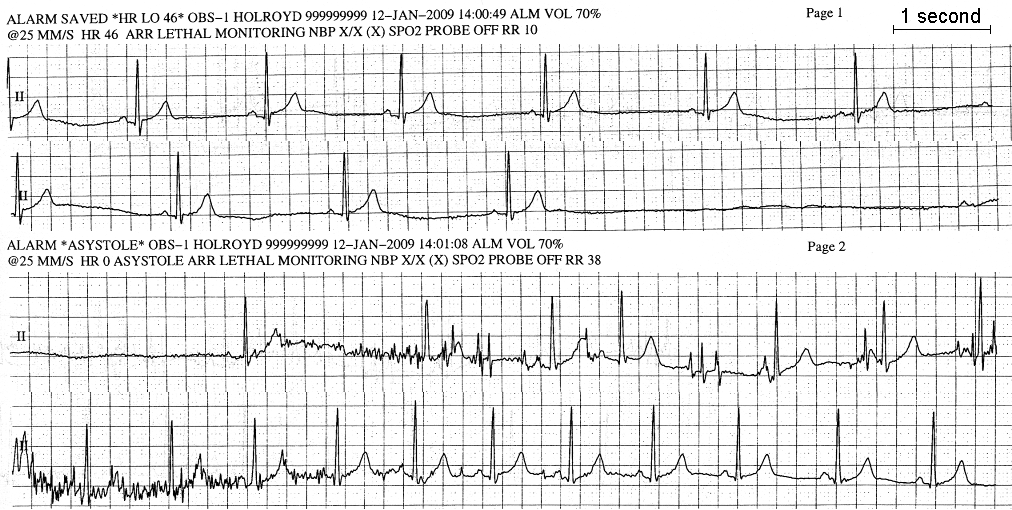
Then abruptly there was no heart beat for about 7 seconds. The EKG graph was "flat-lined". Alarms went off and nurses and doctors quickly gathered from adjacent rooms. My cardiologist (heart doctor) told me to cough, and I did so. I have no memory of this because I had fainted and was unconscious. That jiggled my heart enough for it to try to resume beating. The EKG graph then shows a very irregular period for 11 seconds. After that my heart was briefly at a more rapid rate (70 per minute) before settling down to a normal relaxed rate of 60. My skin had turned white during this. My blood pressure went to zero with the heart stopped but then recovered. My body had been shaking as if in a seizure because of the mixed signals coming from the brain. All of this is what I was told by those in attendance.
When I woke up and was told these things I was very pleased, as a scientist, for a good test with abnormal symptoms being recorded. I would have been disappointed if we had another expensive test that showed nothing wrong. I was fed some orange juice and then some crackers with peanut butter to get some food back into my system. There was some internal shivering which blankets and food helped subside. Recovery took more than an hour before I felt normal again. Gail was allowed back in the room again. Eventually we walked out of the hospital, about two hours after the event, and did errands on the way home.
The heart doctor said that I have "neurocardiogenic syncope" which means something like the signals between the heart and the brain may be somewhat out of order. I am now taking 25 mg of Metoprolol ER (tiny pills) each day. These are a "beta blocker" which ordinarily slows the heart rate so that the brain will not overreact and slow it too much. It also strengthens the communication between the brain and the heart. Since then my pulse rate, measured more than six hundred times at home under a variety of circumstances, is rarely less than 60 and never slower than 53. Further tests confirmed that the pills were adequate and that no pacemaker is needed in my case.
So I was clinically dead for 7 seconds the afternoon of 12 January 2009. I did not have any unusual near-death experience during that brief time. It was total blackout during my faint. However, that was a very pleasant way to die if my heart had not resumed beating. It was sudden and unexpected, with no pain and less than a half minute of warning with mildly odd feelings of the slow pulse rate.
I missed getting to heaven that time to enjoy the rest of eternal life with Jesus Christ. I have no worries about dying again. I just seek to be useful while I am waiting for the ultimate retirement to occur.
For those reading about my unusual experience, you may ponder that any life may end suddenly and without warning. Do you know what will happen to you next? Will it be a transition to life in heaven, or something else? If Jesus were to ask you, "Why should I let you into my heaven?", what would you say? Living a good life is insufficient to make up for the faults that forever eliminate the perfection required for entrance to heaven. Only the righteousness of Jesus can change our status.